CISN - Understanding Your Cancer Pathology Report
| You Are Here: Home > Recently Diagnosed > Your Pathology Report | ||
Understanding Your Cancer Pathology Report |
||
OverviewMaybe you’ve just received your cancer pathology report or you are waiting for your report to be completed. As you might have learned already, a pathology report is a very important document that identifies your cancer diagnosis, including type, stage, and whether or not the disease has spread in the body. This information holds importance because it will likely determine both your cancer diagnosis and treatment plan. Take a deep breath. We know this can be overwhelming. And yet your pathology report offers empowering information toward action. The content allows you and your health care team to develop a targeted plan for your treatments and healing. |
||
|
||
Medical Jargon— More Than Who You AreYour pathology report contains a lot of complex terms associated with your health status. Please remember that you are not your disease or any labels within your pathology report. Beyond your disease type and any related medical predictions, what is your personal will for survival and associated attitudes? These are factors that will have a strong influence on your health and quality of life. |
Statistics
This may not apply to everyone, but certainly many cancer patients read survival statistics associated with their disease after learning their diagnosis from a pathology report. Please remember these numbers are averages based on large populations of varied age groups affected by a myriad of circumstances. Survival statistics associated with your disease type may not apply to you directly. CISN Tip: We recommend looking beyond any survival statistics and realize that you are an individual and nobody can predict your longevity. Pathology 101What is a pathology report? Your cancer diagnosis is determined by examining cells and tissues under a microscope. This information is written up and called your pathology report. |
||
|
||
What information does a pathology report usually include? Although pathology reports are written by physicians for physicians, you may be able to decipher some of the medical jargon provided by the report. The structure and information provided in your pathology report may vary, but the following sections are usually included: Demographics: This section includes your name and date of procedure. You should check that this information is correct to ensure that you have the correct pathology report. Specimen: The specimen section describes the origin of the tissue sample(s) such as what part of your body did it come from. Clinical History: The clinical history section provides a brief description of your medical history relevant to the tissue sample that the pathologist is examining. Clinical Diagnosis (Pre-Operative Diagnosis): The clinical diagnosis describes what the doctors are expecting before the pathologic diagnosis. Procedure: The procedure describes how the tissue sample was removed. Gross Description (Macroscopic): The gross description includes the pathologist’s observations of the tissue sample using the naked eye. It may include size, weight, color or other distinguishing features of the tissue sample. If there is more than one sample, this section may designate a letter or number system to distinguish each sample. Microscopic Description: In the microscopic description, the pathologist describes how the cells of the tissue sample appear under a microscope.
The grade may be described numerically with the Scarff-Bloom-Richardson system (1-3) or as well-differentiated, moderately-differentiated or poorly differentiated. |
||
|
||
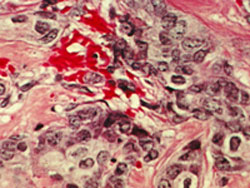
| Image courtesy of the National Cancer Institute (NCI) Visuals Online | ||
Special Tests or Markers: Depending on the tissue sample, the pathologist may conduct tests to further determine whether or not specific proteins or genes are present, as well as how fast cells are growing. Diagnosis (Summary): The final diagnosis is the section where the pathologist concludes the information from the entire pathology report into a concise pathologic diagnosis. It includes the tumor type, lymph node status, margin status and various marker results. This is a very important part of the report and may be the only part you actually read. It will contain everything you need to know and remember. Pathologist Signature: The report is signed by the pathologist responsible for its contents. CISN Tip: Don’t worry about the jargon. Ask your doctor to help explain your pathology report to you. We have included a lot of information here for those who may want it. What is a pathologist?Your pathology report is written by a pathologist. This is a doctor who graduated from medical school but chose to specialize in analyzing tissue under a microscope rather than treating patients. He/she uses all of the information he/she has obtained from various tissue and marker tests, as well as the microscopic examination of the sample. Cytopathologists examine cells from test like FNA’s and pap smears. Surgical pathologists examine cells within tissues from surgical specimens. |
||
Previous Page |
1 2 |