CISN - Personalized Medicine Background Information
| You Are Here: Home > Personalized Medicine > Personalized Medicine & You > Important Background Information (Detail) |
||||||
Personalized Medicine & YouImportant Background InformationWe have provided a brief overview of the terms and science surrounding those terms for those people who want more depth. Tumor markers:Tumor markers (also called biomarkers) are substances found in the blood, urine, stool, or tissue that are produced by cancer cells. Tumor markers may indicate or suggest the presence of cancer. Different tumor markers may be present for different types of cancer. The ideal marker would be a blood test for cancer in which a positive result would only occur only if there were a cancer present. This ideal marker would also indicate the stage of the cancer and possible response to treatment. In addition, it, would be easy to measure.
No current test meets all these requirements. Most tests today have problems with false positive and false negative results. For more information about this click here: |
||||||
| Personalized Medicine & You |
|
| Understanding Tissue Issues |
|
| Ethics | |
| Molecular Diagnostics |
|
Tumor markers can be classified into two groups:
Tumor markers are not always reliable for the following reasons:
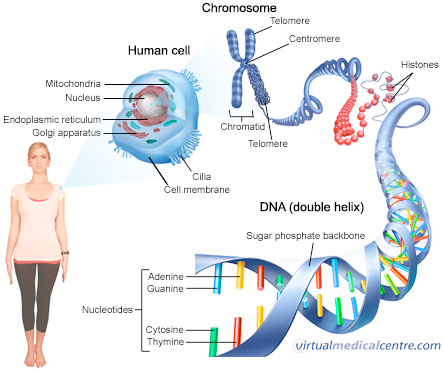
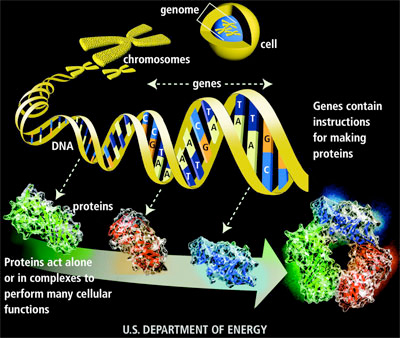
Because abnormal tumor marker levels may only suggest the presence of cancer, other scientific tests are usually required before confirming a cancer diagnosis. GeneticsGenetics is the science of genes and the transmission and variation of inherited traits in other words, the process by which parents may pass certain genetic traits to their children. Characteristics determined by genes range from eye color, hair color, and height to inheritance of or predisposition for specific diseases. Genome refers to an organisms complete set of DNA, including all of its genes. In humans, a copy of the entire genome - which is more than 3 billion DNA base pairs is contained in every cell that has a nucleus. GenomicsGenomics is the study of a persons complete DNA sequence - including genes and noncoding DNA segments in the chromosomes and how those genes interact with each other, as well as the internal and external environments they are exposed to. This includes the study of gene mutations, both those that are passed from parents to children (inherited) and those that happen during your lifetime (somatic). It is these mutations that contribute to the development and spread of cancer.
PharmacogeneticsPharmacogenetics is a specialty field within the study of genomics. It is generally regarded as the study of genetic variation that can affect an individuals responses to certain drugs. Pharmacogenetics uses information about a person's genetic makeup, or genome, to help determine the drugs that are likely to work best for that particular person and/or that may be likely to lead to certain adverse effects. For certain drugs, pharmacogenetics may help to determine whether patients are rapid or slow metabolizers (referring to how long the drug stays in your body) as well as whether they are responders or non-responders (meaning whether the drug works for you). Having the ability to predict a persons individual response to a drug, both in terms of therapy benefit and the likelihood for adverse events, will play a crucial role in:
Deaths from drug side effects are one of the top ten leading causes of death, so this field is very important. EpigeneticsFor decades, scientists and doctors assumed that cancer was caused by irreversible damage to some critical stretch of DNA within one's genome. But in the last few years, a much more complex picture has emerged, one that shows that some cancers are caused by epigenetic changes-tiny chemical tags that accumulate over time and can turn genes on or off rather than mutate them. The word "epigenetic" literally means "in addition to changes in genetic sequence." It is used to refer to any process that alters gene activity without changing mutating the DNA sequence. Experiments show that epigenetic changes, unlike mutations, can be reversed. ProteomicsProteomics is the study of the structure, functions, and interactions of proteins. While genes are the recipe of the cell, containing all the instructions for assembly, proteins are the products of these recipes, functioning as the cellular engines that drive both normal and disease physiology.
A breakthrough in cancer treatment was the discovery that tumors leak proteins and other molecules into blood, urine, and other accessible body fluids. The greatest promise for the early detection and treatment of cancer is to collect such fluids from patients and test them for the presence of cancer-related molecules, called cancer biomarkers or tumor markers.
MetabolomicsMetabolomics is the systematic study of the unique chemical fingerprints that cells leave behind. More specifically, it is the study of how your body responds to drugs, environmental changes and diseases. Metabolomics is an extension of genomics (study of genes) and proteomics (study of proteins). If metabolomic information could be translated into better diagnostic tests, it might have the potential to impact clinical practice, and it might lead to more targeted biomarkers that improves care.
«Click Here to go back to main content. |
||||||||||||||||||||||